Category: Caregiving
Medical ID Wallet Cards vs. Digital Access: Which is Better?
February 11, 2026

The Emergency Question
Picture someone collapsing in a store, unable to talk. Paramedics rush over but need answers. What allergies does this person have? What medications? Any serious health problems? Should these details live on a card in their wallet or sit on their phone?
Here’s the thing: picking just one isn’t the best move.
Medical ID Wallet Cards
Advantages
- Battery? What battery? These cards just work, period.
- First responders get it: About 95% of EMTs know to check wallets.
- Zero connectivity needed: Mountains, basements, middle of nowhere. Doesn’t matter.
- Won’t break the bank: Spend maybe $5-10 once, that’s it.
Disadvantages
- There’s only so much room on a tiny card.
- Wallets get misplaced or left at home sometimes.
- People forget to scratch out old info and add new stuff.
- Cards get wet, fade, or become hard to read after a while.
Digital Smartphone Medical IDs
Advantages
- Room for everything: Write down every single medication and condition.
- Updates take two seconds: New prescription? Changed doctors? Fixed instantly.
- Talks to 911: iPhones automatically send this stuff when someone dials emergency.
- Costs nothing: Already sitting in the phone waiting to be used.
Disadvantages
- Dead phone equals zero help.
- Some paramedics haven’t learned the tricks for every phone type yet.
- Accidents crack screens and destroy phones pretty often.
- Weird fact: Only about 1 in 4 people actually bother setting this up.
The Smart Choice: Use Both
- Medical Alert Jewelry: Get a bracelet stamped with the biggest health concern plus “SEE WALLET CARD”.
- Wallet Card: The most important stuff, right there in physical form.
- Digital Medical ID: Everything else stored on the phone (make sure it shows without unlocking).
- Backup Copies: Stick extras in the glove box, desk drawer, with Mom or a close friend. Consider using a secure digital vault like InsureYouKnow to store copies of medical cards, insurance information, and emergency contacts that family members can access when needed.
Quick Setup
Wallet Card:
- Write down allergies, health conditions, meds, who to call.
- Get it laminated so it lasts.
- Make a few copies.
iPhone:
- Open Health app → Find Medical ID → Turn on “Show When Locked”.
Android:
- Go to Settings → Look for Safety & Emergency → Switch on “Show on Lock Screen”.
Total time needed: about 10 minutes.
Real Examples
- Diabetic collapse: Woman’s wallet card listed her insulin information. Paramedics knew exactly what to do.
- Allergic reaction: Guy’s phone shattered during his fall. Good thing his wallet card mentioned that penicillin allergy.
- Lost senior: Older woman wandered off, couldn’t remember her name. Her iPhone Medical ID had her daughter’s number right there.
Who Needs This?
People dealing with:
- Health stuff like diabetes, seizures, heart trouble.
- Bad allergies that could turn dangerous.
- Pills they take every day.
- Pacemakers, implants, that kind of thing.
Common Mistakes
- Picking one method and ignoring the other.
- Setting it up once and never looking at it again.
- Leaving the lock screen access turned off on phones.
- Keeping it secret from family members.
The Bottom Line
Why choose? Wallet cards save the day when phones quit. Digital files hold way more detail than any card could. Together, they’ve got each other’s backs.
- Money spent: Less than fifty bucks
- Time invested: Ten minutes
- Potential payoff: Might literally save someone’s life
Action Steps
- Today: Get that phone Medical ID set up (takes 5 minutes).
- This week: Print out a wallet card (another 5 minutes).
- Twice a year: Check both and update anything that changed.
When things go wrong, having a backup plan makes all the difference.
Storing Everything Securely
Beyond wallet cards and phone apps, keeping digital copies of medical information in a secure vault ensures family members can access critical details during emergencies. Platforms like InsureYouKnow provide encrypted storage for medical records, insurance policies, medication lists, and emergency contacts. This creates another layer of protection, especially when someone needs to share information with multiple family members or caregivers.
Medical History Cheat Sheet: What ER Doctors Need
February 4, 2026
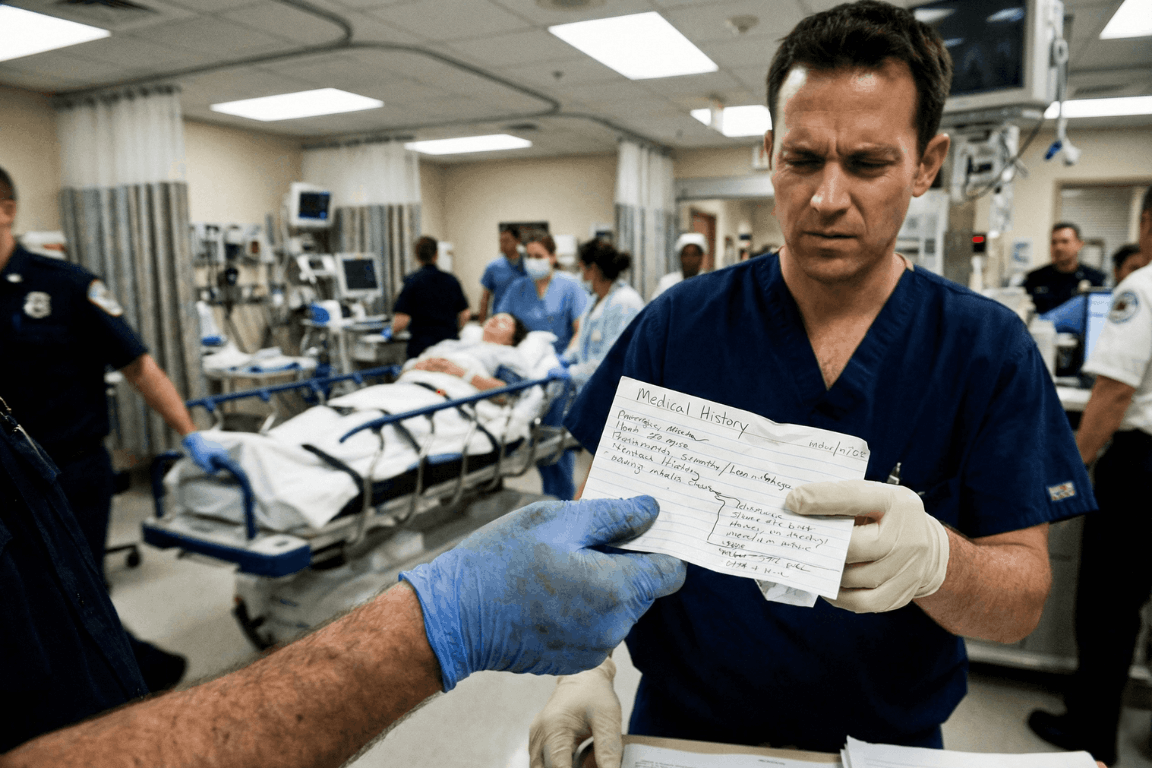
The “Golden Hour” Gap
The Emergency Room is a storm. Noise. Chaos. Speed. Doctors and nurses fight the clock. They chase the “Golden Hour.” That tiny window where fast action beats death.
But silence is the enemy. Ambulances dump patients who can’t talk. Shock takes over. Or they are out cold. In that high-pressure moment, a missing detail, a drug allergy, an old surgery, sends the team down the wrong road. That road ends badly.
Ask any ER staffer. They agree on one thing. A simple “cheat sheet” is the best tool a person can bring through those doors.
Why Memory Fails in a Crisis
People think they will remember. “I know my meds,” they say. They are wrong. Trauma wipes the brain clean. Pain and fear take over. A patient knows they take a “heart pill.” The name? Gone. The dose? Forgotten.
A written paper fixes this. It talks when the mouth cannot. It stops the guessing game between a frantic arrival and safe care.
The ER Doctor’s Wish List: 6 Essentials
What goes on the paper? Forget the thick file. Medical teams want facts. Facts that change the plan right now.
1. The “Big Picture” Demographics
Before the IV goes in, the team must know who they are treating. They need to know who signs the forms.
- Full Legal Name and Date of Birth: This finds old records in the computer.
- Blood Type: Vital for fast transfusions.
- Emergency Contacts: A spouse. A parent. Someone who answers “yes” or “no” to surgery when the patient can’t.
2. The Medication List (Crucial)
This part kills people if it’s wrong. Drug interactions cause huge messes in hospitals. Be exact:
- Prescription Drugs: The name. The dose (like 50mg). The schedule.
- Over-the-Counter (OTC) Meds: Aspirin. Ibuprofen. They seem safe. They aren’t. They thin blood. They hit kidneys.
- Supplements and Vitamins: Herbal pills often fight with anesthesia.
Note: Never write “Take as directed.” That tells the doctor zero.
3. The Allergy Alert
Does the patient hate penicillin? Latex? Contrast dye? The team needs to know. Now. The wrong drug turns a broken bone into a breathing emergency. List the allergen and the reaction. “Penicillin: Hives.” “Peanuts: Throat shuts.”
4. Past Medical History (PMH)
Context is king. A stomach ache in a healthy teen is one thing. In a Crohn’s patient, it’s another.
- Chronic Conditions: Diabetes. Asthma. Epilepsy. High blood pressure. Heart issues.
- Implants: Pacemakers. Metal rods. Artificial joints. The team must know this before an MRI scan starts.
- Past Surgeries: A quick list. “Appendectomy, 2015.” “C-Section, 2020.”
5. Recent History
Sometimes the clue is new. A note about travel, especially overseas, helps. So does a note about recent hospital stays. This helps doctors spot weird infections.
6. Insurance and Directives
Life comes first. But paperwork causes headaches later. List Insurance Policy and Group Numbers. Also, check for an Advance Directive or DNR (Do Not Resuscitate) order. A copy must exist. Otherwise, the patient’s wishes get ignored.
Paper vs. Digital: The Accessibility Problem
Old advice? Keep a card in a wallet. But paper sucks. It fades. It tears. It gets lost. Or it sits in a kitchen drawer while the car crash happens three towns over.
Digital vaults like InsureYouKnow.org changed the game. Storing this “Cheat Sheet” in a secure cloud keeps data safe. It stays ready. A trusted partner pulls up the vault on a phone. Seconds later, the ER team has the facts.
The Final Diagnosis
Being ready isn’t paranoia. It is smart. A Medical History Cheat Sheet takes ten minutes. It pays off in safety. It lets doctors work faster. It stops bad errors. And it gives families peace. They know the health story is clear. Even when the room is silent.
Sandwich Generation Guide: Organize Parents’ & Kids’ Records
January 8, 2026

The Squeeze is Real
The term “Sandwich Generation” sounds polite, almost clinical. But for the millions of adults living it, the reality feels a lot more like a pressure cooker. They are squeezed tight. On one side, there are children needing help with homework, permission slips, and growing pains. On the other, aging parents need support with doctors, medications, and a lifetime of accumulated paperwork.
It is exhausting.
The hardest part usually isn’t the physical caregiving. It is the administration. It is being the unpaid, overworked secretary for two different households. One minute, a parent is hunting for a vaccination card for summer camp; the next, they are frantically searching for Mom’s Medicare supplement number because a receptionist is waiting on the line.
When these worlds collide, chaos wins. Unless, of course, there is a system in place.
Two Households, One Overloaded Brain
The main problem isn’t a lack of effort. It is a lack of centralization. The “Sandwich” caregiver is trying to run two different operating systems at once.
Consider the children. Their documentation is constant and urgent:
- Social Security cards (usually lost in a drawer somewhere).
- Immunization records that schools demand every September.
- Birth certificates for sports or travel.
Then look at the parents. Their paper trail is decades long and much heavier:
- Wills, Trusts, and Deeds (often hidden in “safe” places that no one can find).
- Complex lists of daily medications.
- Insurance policies that need to be renewed.
- The dreaded “In Case of Emergency” contacts.
Keeping the kids’ files in a backpack and the parents’ files in a dusty filing cabinet across town simply doesn’t work. Not in 2026. When an emergency happens, and they always happen at inconvenient times, nobody wants to be driving across town to find a piece of paper.
The “Kitchen Table” Talk
Getting organized starts with a conversation, not a scanner. This is the tricky part. Many adults feel awkward asking their parents about wills or bank accounts. It feels intrusive.
But the conversation doesn’t have to be about control. It should be about safety. The approach matters. Framing it as, “We need to make sure the doctors know what you need if you can’t tell them,” works a lot better than, “Give me your passwords.”
The goal is strictly practical: preventing a crisis from becoming a disaster.
Cut the Clutter: What Actually Matters?
A common mistake is trying to save everything. But honestly, nobody needs to digitize a utility bill from 1998. To survive the squeeze, caregivers need to be ruthless about what they keep.
The “Must-Have” list is actually quite short:
- The Legal Shield: Power of Attorney. This is non-negotiable. Without it, an adult child is legally a stranger to their parent’s bank or doctor.
- The Medical Snapshot: A simple, updated list of what pills they take and who their primary doctor is.
- The Money Trail: Just a list of where the accounts are. Not necessarily the balances, but the locations of the banks and insurance policies.
Stop Relying on Physical Folders
Paper is fragile. It burns, it tears, and most importantly, it stays in one place.
If a parent falls ill while the caregiver is on vacation, that physical folder in the hallway closet is useless. This is why moving to a digital system is the only logical step for a modern family.
Using a secure, encrypted platform, like InsureYouKnow.org, solves the geography problem. It puts the information in the cloud, protected by encryption that is tougher than any lock on a filing cabinet. It means the right information is available on a smartphone, right in the hospital lobby, exactly when it is needed.
Don’t Go It Alone
There is a hero complex in the Sandwich Generation. Everyone tries to carry the load solo. But that is a recipe for burnout.
Once the records are digital, they should be shared. A spouse, a reliable sibling, or a family attorney needs access, too. Modern digital vaults allow for this kind of “trusted partner” access. It ensures that if the primary caregiver gets the flu or gets stuck in a meeting, someone else can step in and handle the situation.
Finding Some Peace
At the end of the day, organizing these records isn’t really about paperwork. It is about buying back time.
Every minute saved by not hunting for a lost insurance card is a minute that can be spent actually being a parent or a son or daughter. The paperwork will always be there, but the stress doesn’t have to be. By merging these two chaotic worlds into one secure place, the Sandwich Generation can finally take a breath.
How to Choose a Medical Power of Attorney and Stay Prepared
November 6, 2025

A few years ago, a close friend of mine went through something that completely changed how I look at “being prepared.” Her dad had a stroke while working in the garden. One minute he was watering plants, the next, he was in the hospital, unable to speak. The doctors were asking who could make medical decisions for him, but no one had an answer. Everyone froze.
It was heartbreaking to watch. Her mom was in shock, her siblings were arguing, and everyone was scared. Nobody knew what he would have wanted.
That day taught me something that I’ll never forget. Planning ahead isn’t just about being responsible. It’s an act of love. And that’s exactly what a Medical Power of Attorney is all about.
What a Medical Power of Attorney Really Means
A Medical Power of Attorney (MPOA) sounds like a complicated legal thing, but it’s actually simple. It’s a document that lets you choose someone you trust to make healthcare decisions if you can’t.
That person, your agent, doesn’t suddenly take over your life. They only step in if you can’t speak for yourself. Their role is to protect your wishes and make sure what you want actually happens.
It’s one of those things we tend to put off, but once it’s done, it brings a quiet kind of comfort. You know things will be okay, even if you can’t explain what you want in the moment.
Why It Matters
If you don’t have a Medical Power of Attorney, hospitals usually turn to whoever’s nearby or follow state laws about next of kin. That can work, but it can also cause a lot of tension. In stressful moments, people don’t always think clearly. They guess, they argue, they panic.
Having an MPOA avoids all that. It gives doctors one clear person to speak with and gives your family direction when things feel uncertain. It’s a simple form, but it can prevent a lot of heartache later.
How to Choose the Right Person
Choosing your agent isn’t about who’s closest to you. It’s about who knows you best. The person you trust most doesn’t have to be family. It could be a friend, a sibling, or someone who simply understands you.
Here’s what to think about:
- Who stays calm under pressure?
- Who knows how you feel about medical care and quality of life?
- Who will listen to doctors carefully and ask good questions?
- Who will do what you want, even if others disagree?
Once you decide, talk to them. It doesn’t need to be formal or serious. Maybe just bring it up during a car ride or while cooking dinner. Tell them how you feel about certain treatments or what kind of care you’d want. These honest conversations matter so much more than any form.
Keeping Your Documents in Order
Once your form is signed, keep it somewhere easy to find. In an emergency, no one wants to dig through stacks of paper.
Here’s what to keep together:
- Your MPOA form (signed and dated).
- A Living Will or Advance Directive describing your medical preferences.
- A HIPAA release form so your agent can speak with doctors.
- Health insurance cards and policy info.
- Emergency contacts for family and doctors.
- Photo IDs for you and your agent.
I like to keep mine in a labeled folder at home and another copy saved online. It’s one of those “just in case” things that saves everyone stress later.
Why Digital Storage Helps
Paper gets lost. It gets packed in a box or tossed by accident. That’s why having a digital copy is smart.
A secure site like InsureYouKnow.org makes it easy to upload and store important documents safely. You can label them, share access with your agent, and know that if you ever need them, they’re right there. It’s simple, private, and safe.
It’s not about being tech savvy, it’s about being practical.
Keep It Updated
Life changes. People move, relationships shift, new doctors come into your life. Once a year, take five or ten minutes to check that your MPOA and other forms are still up to date.
It doesn’t take long, but it gives you peace of mind that everything’s current.
A Final Thought
Setting up a Medical Power of Attorney isn’t about expecting bad things to happen. It’s about kindness, for yourself and the people who love you.
Once it’s done, you can stop worrying. You’ll know that, no matter what happens, your family won’t be left guessing. They’ll already know because you cared enough to prepare.
It’s not just a document. It’s peace of mind, and maybe one of the most loving things you can do.
The Mental Health Gap: What Parents Miss and Teens Need
September 1, 2025

Your teen says they’re fine. But they’ve stopped texting friends, spend more time in their room, and their grades are slipping. Could you spot the signs if they were struggling? Only 58% of U.S. teenagers feel they get the emotional support they need—yet 93% of parents believe they’re providing enough.
Findings like these show that parents may not always realize when their child is struggling. Young people today face different challenges than their parents and previous generations did. More than ever, parents must understand the unique pressures young people are struggling with today.
Challenges Faced by Teens
Nearly 10% of all U.S. kids aged 3 to 17 experience anxiety, while 5% live with depression. A few causes are listed below:
- Many young people are dealing with packed schedules, the pressure to succeed in academics, sports, and extracurriculars, and the uncertainty of what comes after graduation. The pressure to excel can lead to burnout.
- With in-person learning, the fear of school shootings can create a general sense of day-to-day unease.
- Students who remember the pandemic lockdown may have posttraumatic stress from virtual learning and social isolation.
- Social media has introduced young people to near-constant comparison, leading to low self-esteem. Body dissatisfaction is leading to a rise in eating disorders.
- Concerns over climate change can also lead to feelings of hopelessness.
Warning Signs
As a parent, you have a good sense of what your child’s “normal” looks like. In addition to the more striking symptoms, such as mood swings, angry outbursts, or being more tearful than usual, you may notice:
- Changes in eating habits, weight, sleep, or other routines
- Loss of interest in the things they once enjoyed or quitting activities
- Withdrawing from close friends or family
- Academic struggles that seem different or more intense, such as a refusal to complete assignments
- Becoming more visibly worried or expressing constant worry
- Any signs of substance abuse or evidence of self-harm, such as cuts, burns, or bruises
Just because your child exhibits any of these symptoms does not mean they are experiencing a mental health crisis. Biological changes, including hormonal shifts that all teenagers must go through, can affect their mood and school performance.
“It’s kind of hard because these things correlate with puberty,” says Theresa Nguyen, vice president of policy and programs at Mental Health America. “It gets hard for parents because this period of time is so muddy.”
Converse Differently
Checking in with your child is an ongoing process, not a one-time occurrence. Normalizing regular conversations with your child supports their mental health and also gives them the foundation to come to you when they need help.
Kids avoid touchy subjects, especially if they fear being lectured or punished. Make sure your children know they can come to you with anything. Create a safe space for them by remaining approachable and nonreactive. Routine moments, such as car rides or dinner times, can be opportunities for discussion.
Avoid forcing conversations or asking direct questions like, “What’s wrong?” Instead, ask about specific things at school or what they might be looking forward to. They will be more willing to open up if they do not feel interrogated. Try listening more than you speak and resist the urge to give advice immediately.
The goal is not to fix everything for them, but to make sure they know they are supported. “As parents, our instinct is often to jump in with advice, but it’s very rare that that’s what teens are looking for,” says Lisa Damour, a clinical psychologist. “Teenagers often feel supported not through a conversation but through our steady presence. It’s about being around and available.”
Parents can show their teen how to care for their mental health by modeling those healthy behaviors themselves.
- Encourage good physical habits. Eat well and encourage exercise, both of which can be activities you do together. Every family member should have a bedtime and sleep routine.
- Limit screen time and social media. If your teen is resistant, approach it together as an experiment to see if it’s beneficial to take a break.
- Find activities that you enjoy and help them do the same. Ideally, you can find a few things to enjoy together, such as going for walks or watching movies.
“Lead by example,” advises Nguyen.
Your child’s pediatrician can help with any mental health concerns. They can explain treatment options, including medication, and refer you to a specialist for evaluation. Talking with a licensed mental health professional, for instance, can provide teens with a safe and judgment-free zone to process emotions and develop coping skills.
Your child’s care team can develop a crisis plan involving the steps to take if symptoms worsen. There are also courses for parents who want to learn more about mental health first aid. Teens who need to speak with someone immediately may always call The 988 Suicide & Crisis Lifeline or text “TALK” to 741741.
By staying organized, parents can create more time for family. “The single most powerful force for adolescent mental health is strong relationships with caring adults,” says Damour.
Your teen doesn’t need you to have all the answers. They just need to know you’re there every day, without conditions.
At Insureyouknow.org, parents may keep track of their child’s schedule, medical records, and other essential documents.
Intergenerational Care Benefits Everyone Involved
September 29, 2024

September is Intergeneration Month, launched by The Intergenerational Foundation, to connect generations and urge people from varying age groups to socialize. The idea behind recognizing Intergeneration Month each September is to promote learning from each other, such as gaining a better understanding of history and the challenges that separate generations. By connecting with different age groups across generations, unlikely friendships form between those who would otherwise never have communicated with each other.
People balancing raising young children and caring for aging parents may consider looking into what intergenerational daycare can offer. Facilities that provide both child care and senior care are on the rise, and that’s probably because, in addition to being a convenient solution for caretakers, the benefits to each age group are numerous.
If you’re considering Intergenerational Care for your loved ones, here’s everything you need to know.
What is Intergenerational Care?
Intergenerational care centers provide care for both young children and older adults. “It’s also referred to as a ‘shared site,’” says Merle Griff, the director of McKinley Center Intergenerational Project. “In many cases, there’s a senior area on one side of the building, a child care area on the other, and a hallway connecting the two. At various points during the day, they come together,” she says. The care provided can take on several forms, but at the core, it’s a service offered to multiple generations to provide care in one place across age groups.
The benefits of multi-generational care include forming connections between people who have a lot to teach one another and who would have otherwise never been allowed to meet. “It brings younger and older people together to increase social connectedness, enhance well-being for the benefit of all ages, and strengthen the web of support that is so integral to families and communities,” says Sheri Steinig, the director of Generations United. “People of different ages come together to learn, play, grow, and interact in planned intergenerational activities as well as through informal encounters,” she says.
The Different Kinds of Intergenerational Care
While intergenerational care means care across generations, the services provided vary. “There are many settings for intergenerational care,” says Steinig. “There can be programs at community centers and schools or care in daycare centers, retirement communities, nursing homes or assisted living and affordable housing,” she says. You may even provide intergenerational care in the form of a multigenerational household where more than two generations live. One in four American households are already multigenerational.
Intergenerational care centers look more like daycare facilities with adult daycare services or nursing home locations. “Each center is run their own way,” says Griff. “There are typically planned, structured interactions during the day,” she says. Both age groups are usually not combined for the entire day. Daily intergenerational activities may look like a combined sport, arts and crafts activity, comparison presentations between then and now, or even cradling opportunities, where seniors are paired with infants to rock and soothe to sleep. To date, there are fewer care centers than intergenerational programs. While there are only 150 sites across the country, care centers are expected to grow in popularity. For instance, The Mount Intergenerational Learning Center, a Seattle preschool within a nursing home, reports having over 400 children on their waiting list.
Intergenerational care programs are structured pairings between children of various ages and older adults. Programs such as these are designed to foster relationships between youth and seniors. It could be a pen pal program between elementary school kids and seniors, college students visiting nursing homes, multi-age choirs, or veterans going to schools to talk to students about their experiences.
To find a program such as this or a care center in your area, Generations United offers a search tool.
The Benefits of Intergenerational Bonds
Many grandparents live thousands of miles away from their grandchildren while aging adults live several states away from their children. According to a study from the University of California San Francisco, 43% of older adults report experiencing loneliness, and those who feel lonely are at a 59% increased risk of declining health.
That’s when intergenerational care can help. Older adults experience a sense of purpose and renewal after spending time with and helping young people. It helps seniors feel like they are not just receiving care but offering care. “Despite the dementia diagnosis, the maternal and paternal instincts can still kick in, and the seniors feel a sense of purpose,” says Jenna Hauss, the president of ONEgeneration. “They can care for others. They don’t always need to be cared for,” she says.
It isn’t just older generations that benefit from the connection. Children who spend time around older adults have fewer biases around such things as walkers and wheelchairs and become more comfortable with these differences. Multigenerational care promotes sensitivity among both age groups. Parents notice that their children are more empathetic, while older adults experience less loneliness, reduced agitation, and improved overall health.
Intergenerational care addresses two important needs: early childcare and the increasing demand for senior services, but the benefits of this combined service reap rewards far beyond caretaking. Research is proving that both age groups experience different perks from intergenerational connections. If this sounds like it might be the right fit for you and your loved ones, Insureyouknow.org can help you search for care by storing all of your research, financial information, and medical records in one easy-to-review place.
Understanding What Hospice Care Means
July 1, 2024

When treatment for serious illnesses is causing more side effects than benefits, or when health problems become compounded, then a patient and their family members may begin to wonder about hospice. “We recognized as people consider hospice, it’s highly emotional times,” says medical director for Austin Palliative Care Dr. Kate Tindall. “It might include worries and fears.” But one of the things she hears most often from patients and their families is that they wish they had started sooner. Understanding who qualifies for hospice and what it entails is the first part of deciding what might be best for those with terminal conditions.
What is Hospice Care?
Hospice is meant to care for people who have an anticipated life expectancy of 6 months or less, when there is no cure for their ailment, and the focus of their care shifts to the management of their symptoms and their quality of life. With hospice, the patient’s comfort and dignity become the priority, so treatment of the condition ends and treatment of the symptoms, such as pain management, begins. There are no age restrictions placed around hospice care, meaning any child, adolescent, or adult who has been diagnosed with a terminal illness qualifies for hospice care.
An individual does not need to be bedridden or already in their final days of life in order to receive hospice care. Other common misconceptions about hospice care are that it is designed to cure any illness or prolong life. It is also not meant to hasten death or replace any existing care, such as those already provided by a physician.
Determining When it’s Time for Hospice
Establishing care is most beneficial for the patient and their caregivers when it is taken advantage of earlier rather than later. Hospice can be used for months as long as eligibility has been met. Once there is a significant decline in physical or cognitive function, the goal for treatment should become to help that individual live comfortably and forgo anymore physically debilitating treatments that have been unsuccessful in curing or halting the illness.
Both individuals and their loved ones who would benefit from initiating hospice care are often unaware of the services or are uncomfortable asking about them. “It’s a hard conversation to have,” says professor of medicine and palliative care at the Duke University School of Medicine David Casarett. “Many people really want to continue aggressive treatment up until the very end.” While many wait for their providers to suggest it, it should be understood that if eligibility for hospice has been met, an individual and their caregivers can initiate hospice care on their own.
Establishing Hospice Care
In order to qualify for hospice care, a physician must certify that the patient is medically eligible, which means that the individual’s life expectancy is 6 months or less. Typically, the referral to hospice starts with the attending physician’s knowledge of that person’s medical history, while eligibility is then confirmed by the hospice physician. A hospice care team consists of professionals who are trained to treat physical, psychological, and the spiritual needs of the individual, while also providing support to family members and caregivers. Care is person-centered, with the importance being placed on the coordination of care, setting clear treatment goals, and communicating with all involved parties.
Receiving Care at Home
Hospice care is generally provided in the person’s home, whether it’s a personal residence or a care facility, such as a nursing home. “When people are close to the end of their lives, going to the hospital does not make them feel better anymore,” explains professor of medicine at the University of California Dr. Carly Zapata. “Because there’s not necessarily something that we can do to address their underlying illness.” Staying at home allows the individual to be around their personal things and close to their loved ones and pets, which can provide them with comfort during the end of their life.
What Does Hospice Care Include?
Hospice includes periodic visits to the patient and their family or caregivers but is available 24-7 if needed. Medication for symptom relief is administered, any medical equipment needed is provided, and toileting and other supplies such as diapers, wipes, wheelchairs, hospital beds are provided. What may surprise some people is that hospice patients may even receive physical and occupational therapy, speech-language pathology services, and dietary counseling.
If needed, short-term inpatient care may be established for those who cannot achieve adequate pain and symptom relief in their home setting. Short-term respite care may also become available to help family caregivers who are experiencing or are at risk for caregiver burnout. Bereavement care, or grief and loss counseling, is also offered to loved ones who may experience anticipatory grief. Grief counseling is available to family members for up to 13 months after the person’s death.
Paying for Hospice
The first step in finding a hospice agency is to search for ones that serve your county. If there are several options available, then it’s recommended to talk to more than one and see which agency will best fit the patient’s needs. Adequate research should be conducted since not all hospice agencies provide physical and occupational therapy.
Hospice is a medicare benefit that all Medicare enrollees qualify for, but it may also be covered through private insurance and by Medicaid in almost every state. Military families may receive hospice through Tricare, while veterans with the Veterans Health Administration Standard Medical Benefits Package are also eligible for hospice. Hospice agencies will also accept individual self-pay, while there are also non-profit organizations that provide hospice services free of charge.
Discontinuing Hospice Care
Though it is uncommon, if a patient does improve or their condition stabilizes, they may no longer meet medical eligibility for hospice. If this happens, the patient is discharged from the program. Another situation that sometimes arises is when a person elects to try a curative therapy, such as a clinical study for a new medication or procedure. In order to do that, the patient must withdraw from hospice through what is called revocation. Both children and veterans are exempt from being disqualified from hospice care if they choose to also pursue curative treatments. Any person may always re-enroll in hospice care at any time as long as they meet the medical eligibility.
Opting for Palliative Care
Individuals with chronic conditions or life-threatening illnesses may opt for palliative care, which doesn’t require people to stop their treatments. Palliative care is a combination of treatment and comfort care and can be an important bridge to hospice care if patients become eligible. Because transitioning to hospice care can be an emotional choice, palliative care providers often help patients prepare for that. Many people avoid palliative care because they think it is equal to giving up and that death is imminent, but studies show that for many, palliative care allows them to live longer, happier lives. This is due to the benefits of symptom management and spiritual support.
While hospice care can be difficult to accept, it can provide people with the best quality of life possible in their final days, as well as provide their loved ones with valued support. With Insureyouknow.org, you may keep track of all medical and financial records in one easy-to-review place so that you may focus on caring for your loved one, your family, and yourself during this period of their care.
Life After a Stroke: What You Should Know
May 21, 2024
A stroke affects the brain’s arteries and occurs when a blood vessel that brings blood to the brain gets blocked or ruptures. The area of the brain that is supplied with blood by the blocked or ruptured blood vessel doesn’t get the oxygen and nutrients it needs, and without oxygen, nerve cells are unable to function. Since the brain controls one’s ability to move, feel, and think, a stroke can cause injury to the brain that could affect any or all of these functions.
Everyone should know the signs of a stroke and seek immediate medical attention if you think you or someone around you is having a stroke. If you or someone you love has recently had a stroke, then it’s important to understand what happens next.
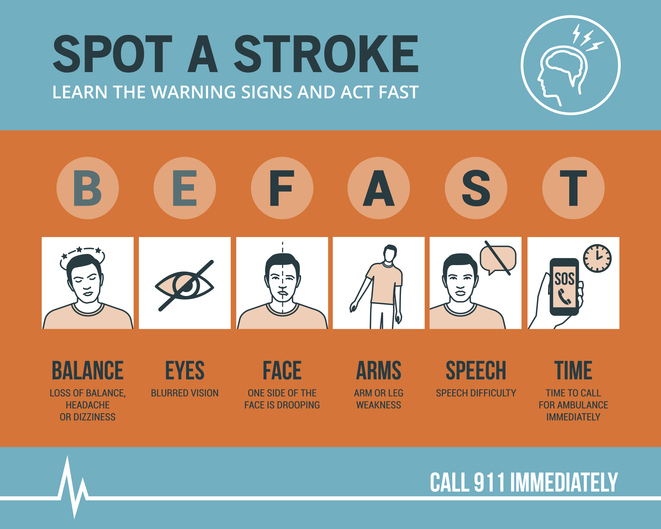
Know the Symptoms of a Stroke and act FAST
The longer the brain is left untreated during a stroke, the more likely it is that someone will have irreversible brain damage. The acronym FAST can help everyone recognize the four main signs that someone may be having a stroke and remember to act fast in seeking medical treatment. That means calling 9-1-1 immediately, as emergency response workers can treat someone on arrival if they think that person is having a stroke.
FAST stands for Facial drooping, Arm weakness, Speech difficulties, and most importantly, Time. If one side of a person’s face is drooping, if the person cannot lift both arms or one arm is drifting downward, and if the person’s speech is slurred or they cannot repeat a simple sentence, then they may be having a stroke. Not all of these signs need to be present to signal a stroke. Just one or two of these symptoms is enough to call 9-1-1, because time is of the essence in the event of a stroke.
Stroke Treatment Begins With Emergency Response Workers
Calling for an ambulance means that the emergency response workers can start life-saving treatment on the way to the hospital. Stroke patients who are taken to the hospital in an ambulance may get diagnosed and treated more quickly than people who wait to drive themselves. The emergency workers may also know best where to take someone, such as to a specialized stroke center to ensure that they receive the quickest possible treatment. The emergency workers can also collect valuable information for the hospital medical staff before the patient even gets to the emergency room, alerting staff of your arrival and allowing time to prepare. All of what the ambulance team can provide saves time in the treatment of stroke, and in the event of a stroke, time is of the essence.
Ischemic Stroke or Hemorrhagic Stroke?
There are two different kinds of stroke, ischemic or hemorrhagic. A medical team will need to determine which kind of stroke the patient is having in order to direct treatment. An ischemic stroke accounts for 87% of all strokes and happens when a blood clot blocks a vessel supplying blood to the brain. Hemorrhagic stroke happens when a blood vessel ruptures and bleeds within or around the brain.
“Fifty percent of strokes present with a clot in a large vessel in the brain, and these don’t respond very well to the old treatment, the IV clot busting medicine,” says M.D. and director of the Sparrow Comprehensive Stroke Center Anmar Razak. “And so nowadays, we do surgery, and what we do is we rush them into the hospital, into the cath lab. We quickly get access through the blood vessels and get up to where the clot is and pull it out.”
With ischemic stroke, the treatment goal is to dissolve or remove the clot. A medication called alteplase or tPA is often administered and works to dissolve the clot and enable blood flow. Alteplase saves lives and reduces the long-term effects of a stroke but must be given to the patient within three hours of the start of a stroke. Then, a procedure called mechanical thrombectomy removes the clot and must happen within six to 24 hours of stroke symptom onset.
For hemorrhagic stroke, the treatment goal is to stop the bleeding. There is a less-invasive endovascular procedure involving a catheter being threaded through a major artery in an arm or leg toward the area of the bleeding in the brain where a mechanism is inserted to prevent further rupture. In some cases, surgery is required to secure the blood vessel that has ruptured at the base of the bleeding.
Rehabilitation After a Stroke
Perhaps the most important part of stroke treatment is determining why it happened or the underlying causes of the stroke. Stroke risk factors include high blood pressure, which weakens arteries over time, smoking, diabetes, high cholesterol, physical inactivity, being overweight, heart disease including atrial fibrillation or aFib, excessive alcohol intake or illegal drug use, and sleep apnea. By making the right lifestyle choices and having a good medical management plan moving forward, the risk of another stroke can be greatly reduced.
That’s because if you have had a stroke, you are at high risk for having another one. One in four stroke survivors have another within five years, while the risk of stroke within 90 days of transient ischemic attack or TIA is as high as 17% with the greatest risk during the first week. This is why it becomes so important to determine the underlying causes of the initial stroke. Your doctor may give you medications to manage a condition, such as high blood pressure, and then recommend lifestyle changes, including a different diet and regular exercise.
Rehabilitation after a stroke begins in the hospital, often within only a day or 2 after the stroke. “There are so many things that patients need to fall into place to be functional and independent again after a stroke,” said Razak. “And they always come down to speed and time.” Rehabilitation can help with the transition from the hospital to home and can help prevent another stroke. Recovery time after a stroke is different for everyone and can take weeks, months, or even years. Some people may recover fully, while others may have long-term or lifelong disabilities. Stroke rehabilitation should be thought of as a balance between full recovery and learning how to live most effectively with some deficits that may not be recovered.
Difficulties from a stroke range from paralysis or weakness on one or both sides of the body, fatigue, trouble with cognitive functioning such as thinking and memory, seizures, and mental health issues like depression or anxiety from the fear of having another stroke. Everyone’s rehabilitation will look different based on their difficulties after a stroke but may include speech, physical, and occupational therapy. Speech therapy helps when someone is having problems producing or understanding speech, physical therapy uses exercises that help someone relearn movement and coordination skills, and occupational therapy focuses on improving daily activities, such as eating, dressing, and bathing. Joining a patient support group may help people adjust to life after a stroke, while support from family and friends can also help relieve the depression and anxiety following a stroke. It’s important for stroke patients to let their medical team and loved ones know how they’re feeling throughout their recovery and what they may need help with.
Stroke rehabilitation can be hard work, but just as in the initial treatment of a stroke, time matters in the possibility of a full recovery. Many survivors will tell you that rehabilitation is worth it and recommend using motivators to achieve recovery goals, such as wanting to see a child’s graduation or returning to working in the garden. With Insureyouknow.org, caretakers may keep track of medical treatments and rehabilitation plans in one easy-to-review place so that they may focus on caring for their loved one during the period of recovery from stroke.
May is American Stroke Month which aims to raise awareness of the second leading cause of death.
Looking after Elderly Parents Remotely
March 1, 2024

Taking care of loved ones without being close by is a challenge. Whether you live a long drive away from aging parents or in another state, long-distance caregiving can become emotionally exhausting. If that sounds like you, know that you are not alone. Nearly 15 percent of caregivers live an average of 450 miles away. If you have recently found yourself looking after your parents from a distance, then here are some simple strategies to help you along the way.
Evaluate Your Strengths and Outsource the Rest
Be honest with yourself about your strengths. Maybe you’re comfortable handling finances but not as comfortable determining medical needs. Pinpointing the areas of need that you’ll be most suitable for is the first step in delegating the rest. You may have siblings who live closer to your parents and are willing to accompany them to their doctor’s visits. Other helpful skills include organization and communication, which could be utilized to organize schedules and communicate with medical professionals and caregivers. Once you determine what you’ll be best at handling, then you can begin to make plans to fill in the gaps.
Create a Team for Support
Speak with the rest of your family and close friends about who can help with your parents’ care. Coordinating with everyone to determine what each person is willing to do will help everyone be on the same page and turn creating a care plan into a team effort. Even if you don’t have any other siblings or family members who are able to help, then you should still meet with your parents and include them in their own care planning. For instance, ask them what you can do that will be most helpful. It’s important to remember that you don’t have to handle everything alone and to try and outsource anything you need help with as much as possible.
Establish Access to Information
Once you determine who the primary caregivers will be and who needs to be in charge of what, then it’s time to make sure those people have access to the appropriate information. Make sure that the person designated to handle bill-paying and account management on behalf of your parents has the ability to do so. Establishing the rights to have medical information released to caregivers as well as decision-making rights is another imperative. This can also be a legal issue down the road, so making sure that you or another trusted party is the power of attorney, who is appointed to make financial and medical decisions, will need to be determined.
Revisit Living Arrangements
Sometimes a loved one’s health requires them to be closer to you. If it’s possible to relocate to where they live or have them move in with you, then that may be something worth exploring. If it’s not possible to live together, then senior living communities have the upside of being able to provide 24/7 care. Many older people don’t require full-time care though, so if relocation isn’t feasible, then hiring a home care aide or personal care assistant is another option.
Schedule Regular In-Person Visits
If you cannot live close to your parents, then making plans to see them will accomplish several things. First, you’ll instantly alleviate some of the caregiver guilt you may be experiencing just by knowing when you’ll be able to visit them next. Second, you’ll be able to check on them in-person, as you may not have an accurate assessment of their condition and needs from a distance. “It’s hard keeping a handle on their health, how they’re doing, physically, mentally, psychologically and emotionally, when you’re not there,” says Amy Goyer, AARP’s family and caregiving expert. “Isolation is a big thing and they can tell you, oh, I’m doing fine and everything on the phone, but is that really what’s happening?”
Lastly, but most importantly, you’ll be able to spend some much-needed quality time with your parents when visiting. If you are not the primary caregiver, then coordinate with them on when the best time to visit is and offer them a break. Plan in advance what you can do when you’re there to help out. Then speak with your parents about what they would like to do with you during your visit. Since visits can go by quickly, especially when there is so much to do, set priorities ahead of time about what’s most important once you’re there.
Remain Connected When You’re Apart
Schedule regular phone calls with your parents and ask for updates from their caregivers. With their permission, you may even choose to attend their telehealth visits and doctor’s appointments virtually. “The frequency of contact is dependent on the type and level of care needed,” says Iris Waichler, author of Role Reversal, How to Take Care of Yourself and Your Aging Parents. “It should be a collaborative decision, if possible, rather than a unilateral mandate from the caregiver.”
Regular communication can keep your bond with your parents strong, as long as it remains an enjoyable experience for all of you.
Take Care of Yourself as Well
Caregiving can come with a heavy emotional load. It will become just as important to check in with yourself in your new role as caregiver. “Caregivers may often feel like they can do more and this can cause ruminating thoughts,” says Brittany Ferri, geriatric care occupational therapist. “In this instance, they may benefit from practicing positive self-care and self-talk along with their loved one to keep the lines of communication open while relieving stress.”
It’s hard to be a good caregiver, when you’re running on empty, so taking care of yourself as well is just as important as taking care of those depending on you. Show yourself compassion, make sure you’re recharging, and be kind to yourself.
Insureyouknow.org
While it can be a challenge to care for your parents from a distance, that doesn’t mean it’s not manageable. By planning ahead and creating a care team, you can make sure your parents are cared for even when you can’t be close at all times. Insureyouknow.org can help you compile care plans, schedules, financial information, and medical records all in one place. Then you can rest easy that you have a plan set in motion, ensuring that your parents will be well-taken care of.
